Services

Services
Bad breath can often stem from the infection of periodontal disease. In order to stop this problem, patients need to see an periodontist and then get in the habit of good brushing and flossing.
That being said, please be aware that the vast majority of people with chronic bad breath have healthy gums. It’s been proven that halitosis (bad breath) is caused by bacteria on the back of the tongue, breaking down mouth proteins into odor-causing compounds.
Though vigorous tongue scraping will help with bad breath, it’s still not enough for some people.
We advise patients dealing with periodontal disease to know the anatomy of the tooth-supporting structures. These include the periodontal ligament which attaches the tooth root to the socket, as well as the gum tissue which attaches to the bone and surrounds the tooth like a collar.
Depending on the situation, periodontal disease can affect one tooth or many teeth. When gum inflammation is caused by the release of toxins from the bacteria in plaque, the infection begins.
The gums then start to swell, appear puffy and bleed easily. In this stage, also called gingivitis, the patient experiences little discomfort. These symptoms are reversible with regular dental cleanings and proper oral hygiene habits.
Untreated gingivitis has the potential to advance to periodontitis. Plaque gradually hardens to form tartar and grows below the gum line, detaching the gums from the tooth. Bone resorption consequently occurs, as well as the formation of infected pockets. Pockets slowly deepen while more gum and bone tissue are destroyed. Patients experience bleeding gums, a bad taste in the mouth, halitosis and abscesses. Teeth may even have to be removed if they become too loose.
Remember that gingivitis and early periodontitis can be easily treated with scaling and root planing. These methods remove plaque and tartar from deep pockets while also smoothing the root surfaces.
Even though many patients don’t require any further active treatment, the majority will require ongoing maintenance therapy to sustain periodontal health. Please be aware that non-surgical therapy does have its limitations and that surgery may be the only option in certain cases.
The most common periodontal surgery options are pocket reduction procedures and regenerative procedures. Both may be advised when root planing and scaling do not help in the restoration process.
This involves the folding back of gum tissue, in addition to the removal of disease-causing plaque and tartar. Irregular surfaces of the damaged bone may be smoothened to allow the gum tissue to better reattach to healthy bone. Sutures are then used to secure the gum tissue at its new position.
Eliminating bacteria alone may not be sufficient to prevent recurrence of periodontal disease. Since deeper pockets are more difficult for you and your dentist to clean, it’s important to reduce them. Combining this proper oral hygiene and regular cleanings will increase the chances of keeping your natural teeth.
If a defect exists in the bone, a bone graft may be placed to stimulate new bone formation.
Natural or synthetic bone can be used for regeneration. At times, specialized membranes can be an option to prevent the gum tissue from creeping in between the tooth and bone.
This then creates a regeneration of new bone and periodontal ligament.
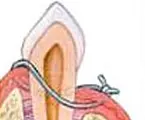
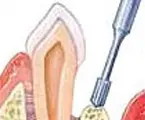
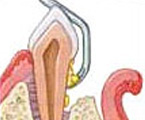
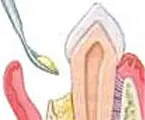
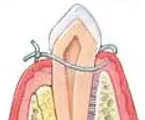
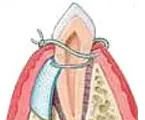
Regenerative Procedures
Cosmetic Surgical Procedures
Crown lengthening involves the removal of gum tissue; bone or both expose a tooth’s structure more sufficiently.
The procedure is done when a tooth breaks off at the gum line, or a filling or crown falls out of a tooth with extensive decay underneath. Your dentist may need to expose more of the tooth by removing some tissue and bone.
Occasionally, where an unusually large amount of gum tissue shows around the upper teeth (called a gummy smile), crown lengthening may be used.
Done under local anesthesia, incisions are made to reflect the gums away from the teeth. Doing this provides access to the roots of the teeth and surrounding bone. In most situations, your periodontist will need to remove some bone from around the roots of the teeth. By using a combination of rotary and hand instruments, the bone is removed and the gum tissue is secured with sutures.
Since the gums are now sitting at a lower level than before the surgery, your teeth will look longer and more attractive. Sometimes, an intraoral bandage will be used to cover the site and help protect it during healing. We will remove any temporary crowns prior to the procedure and replace them afterward.
Soft tissue grafts help treat gum recession and can improve the esthetics of one’s gum line. Aggressive tooth brushing, periodontal disease or clenching of teeth can all play a role in gum recession. Exposed tooth roots, the byproduct of gum recession, gives you an older look and causes sensitivity to cold liquids and foods.
Soft tissue grafts can cover roots or develop gum tissue where needed. To complete this procedure, your periodontist takes gum tissue from your palate or another donor source to cover the root. Not only can a soft tissue graft further reduce recession and bone loss, but also protect the root from decay and heightened sensitivity.
Crown Lengthening
Soft Tissue Grafts
Please see the Surgical Periodontal Treatment page for
additional information.
Regular follow-up care is essential to maintaining periodontal health. Your periodontist will discuss with you how often follow-up care appointments need to be scheduled. Periodontal maintenance helps eliminate bacterial plaque, eases the healing process and prevents further bone destruction.
Fee Schedule
In compliance with Colorado state law, the fee schedule for the 15 most
common codes our offices use for a cash patient are: